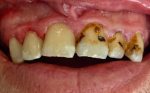
Tooth Abscess
Antibiotics
Tooth abscess antibiotics are an essential part of treatment for an infected tooth. Antibiotics for tooth infections are very effective, and the most commonly prescribed antibiotic these days is probably Amoxicillin, a type of penicillin. It's usually called Amoxyl. More details further down this page.
BUT you don't ALWAYS need antibiotics, and these days we are trying to cut down on antibiotic prescribing due to bacteria becoming resistant. If it's possible for your dentist to drain an infection, either by making a small hole in the tooth or else by making a small incision in the gum to let the pus out, then the infection has a way out, and you may not need antibiotics.
 antibiotics will help
antibiotics will helpTooth Abscess Antibiotics
The discovery of the first antibiotic - penicillin - by Nobel Prize-winner Alexander Fleming created a revolution. As Woody Allen said, "I wouldn't want to have lived in any time period before the discovery of antibiotics".
When you think about it, he's right! Before antibiotics came along, many people died from simple infections that would be treated very easily today
ONE THING to remember, though, is that we have an increasing problem of bacteria becoming immune to our antibiotics for tooth infections.
ANTIBIOTIC RESISTANCE.
Potentially, this is a very serious problem, because it means that in the future, a simple infection might kill you if the bacteria responsible have become immune to antibiotics.
The problem of some types of bacteria developing immunity (or "resistance") to common antibiotics has developed gradually over recent years, due to doctors and dentists "over-prescribing". Over-prescribing happens when a doctor or dentist prescribes antibiotics for a suspected infection, when either there is NO infection OR the infection would settle down anyway without antibiotics.
While there is A LOT of research being done into new, alternative antibiotics, we can all help to reduce the problem of antibiotic resistance by only taking current tooth abscess antibiotics when we are SURE that there is an infection caused by bacteria, with a swelling, difficulty opening your jaw, or a raised temperature.
THERE ARE ALSO NEW PRESCRIBING RECOMMENDATIONS! Recent studies (in late 2017) have shown that SHORT courses of antibiotics (ie. 3 to 5 days) are just as effective as longer courses (ie. 7 to 10 days). AND taking antibiotics for longer than 3 to 5 days means that you are MORE LIKELY to get an antibiotic-resistant infection!
The report recommends only taking antibiotics for as long as you still have symptoms. As soon as you feel things are back to normal, you can STOP taking the antibiotics.
5 Best Tooth Abscess Antibiotics For Tooth Infections
BUT LET"S GET to that list of antibiotics for a tooth infection;
Here is a list of the most widely-used tooth abscess antibiotics:
1. Penicillin V. (Also called "Pen Vee") This is a form of penicillin that has been around for quite a while, but it is still very effective. It works against a relatively small number of bacteria types, but they are the ones that are most commonly involved in dental infections. Because it is a "narrow spectrum" antibiotic, it is less likely to cause a general "antibiotic resistance".
BUT it's very important to take a high enough dose for it to work properly. It's only effective if it has a high enough concentration in your blood stream to kill bacteria. At lower blood concentrations it can only inhibit the bacteria from multiplying, rather than killing them.
 Alexander Fleming
Alexander FlemingTo keep the level of Penicillin V in your bloodstream high enough, it must be taken in 4 doses spread out over the day. The normal dose is 250mg every 6 hours.
If it is taken less frequently, say once every 8 hours, the blood concentration may dip below the effective bacteria-killing level for an hour or so before the next dose is taken. So one dose every 6 hours is needed to make sure the bacteria are being killed.
Unfortunately, people tend to miss one of the doses during the day, because they forget or they are busy. This means that Penicillin V doesn't always work quite as well as it should do. Most dentists will now prescribe a more modern form of Penicillin - Amoxicillin. Read on!
2. Amoxicillin is different to Penicillin V in that it is well absorbed in the stomach when taken in capsule form by mouth, and even better if you have something to eat when you take the capsule. It's also "broad spectrum", i.e., effective against many types of bacteria. So whatever bacteria is causing your tooth infection, Amoxicillin will probably be effective.
It's one of the best tooth abscess antibiotics. An extra plus point is that you only need to take three doses a day, (500mg every 8 hours) so it's easier to keep track and take the course correctly. You're less likely to miss a dose, as there's only 3 a day to remember. For most folk, that's one capsule after breakfast, one before bedtime, and one somewhere in the middle of the day.
HOWEVER, the recommended dose DOES seem to vary from country to country. In some countries, the dose is 250mg taken FOUR times a day. (The same as for Penicillin V). In other countries, the recommended dose is 500mg, taken THREE times a day! And this has been shown to be very effective.
So, depending where you live and how up to date your doctor or dentist is, the DAILY dose seems to be between 1000mg and 1,500mg. This is divided over 3 to 4 intakes per day.
 Clamoxyl
Clamoxyl2b. Clamoxyl is a mixture of Amoxicillin and clavulanic acid, which makes it resistant to breakdown by certain bacteria, and so even more effective than straight Amoxicillin. It's a pretty heavy hammer, and is effective against a wide range of bacteria, but it can knock out some of the "good guys" too.
We all have "normal" bacteria in our mouths and stomachs which are essential to normal function. Sometimes these good bacteria can be affected by antibiotics prescribed for infections.
Personally, I think Clamoxyl (Amoxicillin combined with clavulanic acid) is too powerful and unnecessary for most dental infections. It should really only be prescribed if you have had a swab or sample of the infection sent to a laboratory for testing, to see if the infection is being caused by a bacteria that can break down plain Amoxicillin.
5 Best Tooth Abscess Antibiotics
3. Metronidazole. This is marketed under the name Flagyl in most countries. It is very effective against certain types of bacteria that can cause gum infections. It is important to avoid alcohol while taking Metronidazole, as it may cause serious stomach upsets. This won't harm you in any way, but you may end up vomiting, which means you lose some of the antibiotic, and it won't be as effective.
Metronidazole is particularly good for infections under the gum around the neck of the tooth or a dental implant infection. It is effective against bacteria that do not need oxygen. In fact, these bacteria are INHIBITED by oxygen.
These are called "anaerobic" bacteria. They frequently cause dental infections in the gum over a wisdom tooth that is just poking through the gum a little; anaerobic bacteria can also cause a severe infection that usually appears between the lower front teeth called Acute Ulcerative Gingivitis.
For more stubborn infections, Metronidazole can be taken at the same time as Amoxicillin. Working together, the two antibiotics have a synergy which produces an effectiveness much greater than could be expected from just adding the two together! Tooth infections don't stand a chance against this powerful combination!
3b. In Spain, there is a ready-made Metronidazole combination that uses Spiramycin as the second component. Like Amoxicillin, it is supposed to act synergistically with Metronidazole to produce a greater effect than the 2 products taken separately!
2022 update - I recently cracked a back molar tooth on a peppercorn. Ouch! After root canal and a gold crown, I had some peace for about 3 years. Then the abscess flared up. I started on Amoxicillin, with little improvement. Then I switched to Clindamycin, also with only slight improvement;
Now I was beginning to suspect the worst. After a 2 week break to allow my stomach bacteria to normalize, I went on a course of the Metronidazole + Spiramycin combo,called Rhodogil in Spain. After 3 days there was little change, so I ADDED Amoxicillin into the mix as well. This produced a gradual improvement, but not good enough for me to be able to chew with the tooth.
 Rhodogil
Rhodogil Rhodogil
RhodogilRegretfully, I had to face the fact that tooth abscess antibiotics were not going to be the "magic bullet", and I had to have the tooth extracted. This just goes to show that not even the best abscess antibiotics can save the day.
5 Best Tooth Abscess Antibiotics
4. Erythromycin. This is an older antibiotic, but it is still in use, and very effective where you might be allergic to the penicillins. However, it may cause various types of stomach upset, and so is usually kept "in reserve". As a tooth abscess antibiotic, it's unusual to prescribe this one. I can't remember the last time I prescribed it.
 Clindamycin capsules
Clindamycin capsules5. Clindamycin is the 500lb. gorilla of tooth abscess antibiotics used in dentistry. It penetrates bone extremely well, and for this reason is normally given in much lower doses than other antibiotics.
The usual dose is 150mg, taken FOUR times a day. This makes it very good for infections within the bone, such as a tooth extraction infection. However, it does have a very small risk of causing a potentially serious stomach condition.
For this reason, it is usually kept in reserve as an "antibiotic of last resort". Having said that, it is becoming increasingly more widely used.
Clindamycin is also an alternative antibiotic if you are allergic to penicillin.
Tooth abscess antibiotics are also used in other areas of general medicine. They just happen to be particularly effective against the bacteria that commonly cause dental infections.
All antibiotics for tooth infections work in one of 2 ways; either they kill the bacteria outright, or else they slow down or stop the bacteria from multiplying, and so give your own immune system a chance to work.
The ones that kill bacteria are called "bacteriocidal", and the ones that stop bacteria multiplying are called "bacteriostatic". You might think that the best antibiotics for tooth infections are the bacteriocidal ones, but this isn't always true. Clindamycin, for example, is bacteriostatic, but extremely effective! The effectiveness of an antibiotic for dental use depends also on how well that antibiotic penetrates the area it needs to get to.
To get the best results, you must always take your antibiotics exactly as directed by your health care professional.
Remember to check out my top recommended electric toothbrush, which has the best performance and a great price at Amazon - the Cybersonic 3 brush.
Tooth Abscess Antibiotics - Side Effects
Side effects of antibiotics are the unwanted effects that antibiotics may cause, in addition to the beneficial effects of eliminating bacteria. Unwanted side effects include;
- Allergic reaction to the antibiotic
- Stomach upsets, including discomfort, pain, and diarrhea.
- A sore tongue.
Allergic reactions can be very mild, such as a slight itchy skin rash, typically on the chest and the inside surfaces of the forearms.
Moderate allergic reactions involve nausea and/or diarrhea.
Severe allergic reactions may be life-threatening if anaphylactic shock is triggered. This involves difficulty breathing, severe nausea or vomiting, swelling of the neck and tongue, and fast heart rate. You should call 911 immediately.
Stomach upsets can also be caused by the alteration in of the balance stomach bacteria. Antibiotics are aimed at dealing with bad bacteria that are causing an infection, but they will also affect some of the normal bacteria that live in our stomach and intestines. This can cause a bit of an upset stomach, but things return to normal within a few weeks of finishing the course of antibiotics.
A sore tongue is less commonly reported, but I believe that it happens quite a lot. It's called "antibiotic sore tongue", and your tongue looks red and inflamed, but it is NOT puffy nor swollen. It's just red, and tender, particularly to food and drinks that are acidic. This settles down after you stop taking the antibiotics.
I hope you have found my list of the 5 best tooth abscess antibiotics useful. Here is another article about tooth abscess antibiotics at Medscape.